4 Ways Diabetes Can Affect the Health of Your Eyes
Eye health is always important, but diabetics face unique challenges that many other people don’t. Diabetic eye disease can develop in multiple ways and each one affects your vision differently. Knowing the ways diabetes can affect the health of your eyes can help you understand why comprehensive eye exams are so important to your eye health.
In this blog we will cover:
- What is diabetic eye disease
- Comprehensive eye exams in Knoxville, TN
- How diabetics can affect the health of your eyes
What Is Diabetic Eye Disease?
Diabetic eye disease isn’t one single disease but rather an umbrella term for a group of diseases you can develop due to diabetes. Common diabetic eye diseases include:
- Diabetic retinopathy
- Diabetic macular edema
- Glaucoma
- Cataracts
Diabetes interferes with your body’s ability to either produce insulin or control blood sugar ( glucose ) levels effectively. Having too much glucose in your blood can seriously damage multiple parts of your body, including the heart, kidneys, and blood vessels. Diabetes can also damage the blood vessels in your eyes leading to vision problems.
Fortunately, it’s estimated that around 90% of diabetes-related vision loss can be prevented. A key factor is early detection with comprehensive eye exams. These exams allow our team of ophthalmologists to take a deeper look at the inner structures of your eyes and detect problems early on before they have a chance to develop into major issues in the future.
To learn more about the connection between diabetes and eyesight from an ophthalmologist, click here !
Comprehensive Eye Exams in Knoxville, TN
Comprehensive eye exams aren’t like the vision screenings you may have had as a child. Those tests were designed to catch vision problems in children that prevent them from doing well in school. They aren’t designed to give eye health experts the same level of knowledge about the eye that comprehensive eye exams do.
With comprehensive eye exams, eye doctors can view parts of your eyes that can alert them to other health issues. For instance, they can spot the effects of diabetes on blood vessels within the eye and monitor their progress. In some cases, your eye doctor may even be the first person to spot these signs so you can get the treatment you need.
Other health problems we can catch with comprehensive eye exams include:
- Cataracts
- Glaucoma
- Hypertension
- Autoimmune diseases
- Macular degeneration
These and other problems can have a major impact on your daily life. Cataracts, glaucoma, and macular degeneration can reduce your vision and even lead to blindness if left untreated. Hypertension and autoimmune diseases can interfere with your heart, vascular, and overall health. With comprehensive eye exams, you can be alerted to these issues and get treatment.
Click here to learn more about where to get comprehensive eye exams in Knoxville!
How Diabetes Can Affect the Health of Your Eyes
Diabetic eye diseases can come in different forms. Some are directly related to being diabetic, such as diabetic retinopathy and diabetic macular edema. Diabetes can also increase your risk of other eye diseases, which is the case for glaucoma and cataracts. By working with your doctor, you can help mitigate diabetic eye problems and preserve your vision for years to come.
1. Diabetic Retinopathy
Diabetic retinopathy is caused by the blood vessels in the retina becoming damaged. Located on the back wall of your eye, the retina is a lining of cells responsible for sensing light and sending signals to the brain to create the images that you see. This can eventually result in permanent loss of vision if not treated immediately.
What Causes Diabetic Retinopathy?
Diabetic retinopathy is caused by having high blood sugar levels. Over time, the tiny blood vessels in your eyes can get blocked and cut off blood flow from your retina. The eye’s natural response to this problem is to create new blood vessels to replace the blocked ones. Unfortunately, the new blood vessels will malfunction and leak fluid into the rest of your eye.
Diabetic retinopathy comes in two forms: early and advanced. Most people with the condition have early diabetic retinopathy , also known as nonproliferative diabetic retinopathy (NPDR). This simply means that the body isn’t growing new blood vessels in the eyes to replace the ones that have become blocked.
During early diabetic retinopathy, the walls of the smaller blood vessels in your eyes begin to weaken. Tiny bulges then begin to form with fluids starting to leak as the walls of the blood vessels weaken. Larger blood vessels in the retina can also begin to swell and take on irregular shapes. These problems will only become worse as more blood vessels are blocked.
If left unchecked, early diabetic retinopathy can turn into advanced diabetic retinopathy . This form of the disease causes the damaged blood vessels to close off and new ones to grow in their place. The problem is that these new blood vessels are much more fragile, causing more fluid leakage into the jellylike substance that fills your eyes, known as vitreous .
The growth of new blood vessels can cause scar tissue to develop leading to a retinal detachment. The new vessels can also prevent fluids from leaving the eye and increase pressure inside of it. Over time, this pressure can damage the optic nerve which is responsible for transmitting images from the eye to the brain, leading to glaucoma.
Diabetic Retinopathy Symptoms
Early diabetic retinopathy, also known as background diabetic retinopathy , usually has no symptoms. This means that you may have the disease without realizing it, which is why regular comprehensive eye exams are so important. They allow our eye doctors to catch it early and provide treatment in order to slow its development.
Symptoms start to become apparent as the disease progresses into advanced diabetic retinopathy. At this stage, you may begin noticing:
- Floaters in your field of vision
- Blurry vision
- Dark or blank spots
- Decreased night vision
- Faded colors
Be sure to talk to your eye doctor if you experience any of these symptoms. It can be difficult to restore your vision once advanced diabetic retinopathy has set in, but treatments are available to preserve the vision that you still have.
Diabetic Retinopathy Treatment
Treatments for diabetic retinopathy can vary based on the type you have and how severe it is. The condition can’t be reversed or cured, but its progression can be slowed with proper treatment. Your eye doctor will keep track of your progress through comprehensive eye exams.
Treatment may not be necessary for mild to moderate cases of early diabetic retinopathy. With that said, your eye doctor will still want to see you regularly to monitor your progress. You can work with a diabetes specialist (endocrinologist) to help manage your diabetes. They can help you manage your blood sugar to slow the spread of this diabetic eye disease.
Treatment for advanced diabetic retinopathy can be more involved. Depending on your specific problems, your eye doctor may recommend:
- Medication injections into the eye. Known as vascular endothelial growth factor inhibitors , these medications are injected into the gel-like substance that fills your eye and gives it shape. They help to prevent new blood vessels from growing and reduce fluid buildup. These injections will need to be repeated on a regular basis in order to keep working.
- Photocoagulation. This is a form of laser treatment also known as focal laser treatment . It helps reduce or even prevent blood and other fluids from leaking into your eyes. For this procedure, your ophthalmologist uses a laser to burn the abnormal blood vessels.
- Panretinal photocoagulation. This is another form of laser treatment that uses a scatter laser to shrink the abnormal blood vessels. Your doctor will focus the laser to focus scattered laser burns on the retina. This causes the abnormal new blood vessels to shrink and scar.
- Vitrectomy. Vitrectomy is a surgical process where a tiny incision is made in the eye to remove blood from the gel-like substance inside. Your eye surgeon will also remove any scar tissue that may be tugging on the retina that could lead to retinal detachment.
To learn more about diabetic retinopathy, click here !
2. Diabetic Macular Edema
As early diabetic retinopathy develops, patients can develop another issue known as diabetic macular edema . It occurs when fluids from the damaged blood vessels make their way into the macula , which is the center of the retina and has a very high amount of photoreceptor cells. It’s responsible for the central vision that allows you to see things that are directly in front of you.
Neither diabetic macular edema nor early diabetic retinopathy result in major vision loss. However, diabetic macular edema can cause blurred vision for those with the condition. This can make it difficult to drive or perform other daily tasks confidently and safely. Regular visits to our office are the best way to stay on top of your symptoms and get the treatment you require.
Diabetic Macular Edema Symptoms
Diabetic macular edema and diabetic retinopathy share similar symptoms since they both affect the retina. This includes:
- Blurry vision
- Double-vision
- An increase in eye floaters
It’s very important to have yearly comprehensive eye exams if you are diabetic. They give our eye doctors an opportunity to see if you are developing symptoms of diabetic macular edema and develop a treatment plan.
Treatment for Diabetic Macular Edema
As with symptoms, diabetic macular edema and diabetic retinopathy treatments share a lot in common. Both make use of vascular endothelial growth factor inhibitor injections as well as laser treatment.
Treatment for this diabetic eye disease also includes corticosteroids , a type of steroid that is injected into the eye. This may involve injecting medicine directly into the eye or injecting a steroid eye implant. In the latter case, medication is released over time in order to reduce the effects of the eye disease and improve your vision.
3. Glaucoma
Advanced diabetic retinopathy can eventually result in glaucoma if not treated immediately. The exact cause of glaucoma is unknown although experts have noted that it’s often connected to an increase in eye pressure. Glaucoma affects your vision by damaging the optic nerve which connects the eye to the brain. Over time this can cause you to lose your peripheral vision.
A healthy eye produces a watery liquid known as aqueous humor that flows through the eye to provide nutrients and help maintain consistent eye pressure. Glaucoma occurs when the aqueous humor doesn’t drain properly and instead acts as a sink, causing the eye’s natural drainage systems to become clogged.
This causes pressure within the eyes ( intraocular pressure ) to increase, damaging nerve fibers and resulting in reduced vision or even blindness. Open-angle glaucoma is the most common form of glaucoma and accounts for 90% of glaucoma cases.
It’s also the most common type for diabetics as they are twice as likely to develop it as non-diabetics. Similarly, those with open-angle glaucoma are much more likely to develop diabetes than those without it. It increases your eye pressure by gradually clogging drainage canals despite the angle between the cornea and iris remaining open.
Neovascular glaucoma is a much rarer form of glaucoma. However, it is often found along with other health issues, diabetes being the most common. This form of glaucoma is associated with the abnormal blood vessels that develop during advanced diabetic retinopathy. The new vessels can grow on the iris, release fluid, and result in increased eye pressure.
Glaucoma Symptoms
Glaucoma symptoms can vary depending on the type you have. Open-angle glaucoma is the most common form even among diabetics. The main symptoms of this type of glaucoma are:
- Reduced peripheral vision
- Tunnel vision
Open-angle glaucoma attacks your peripheral vision making it harder to see out of the corners of your eyes. It can also affect your central or “front” vision, as well. Glaucoma can manifest itself as blind spots or patches in your side or front vision, alerting you that something is wrong. This can eventually result in tunnel vision at the advanced stages of the disease.
Glaucoma Treatment
Glaucoma can be treated in a number of ways including eye drops, oral medications, surgery, and other forms of therapy. Eyedrops are often the first step in glaucoma treatment to help control eye pressure. There is a wide variety of glaucoma eye drops available and your eye doctor can help determine which is best for you.
Unfortunately, eye drops alone aren’t always enough to control your eye pressure. In this case, oral medications can be prescribed to bring it down to a desirable level.
Surgical procedures and other treatments include:
- Laser therapy
- Filtering surgery
- Drainage tubes
With laser therapy , your doctor aims a small laser beam at the clogged channels in your eye to promote the flow of fluids. Filtering surgery involves the creation of a new opening for fluid to move through. Drainage tubes can be surgically implanted to drain excess fluids.
Click here to learn more about glaucoma and how it affects your eyesight!
4. Cataracts
Cataracts are the leading cause of blindness across the globe and can be worsened by diabetes. They grow slowly on the lens of your eye, often with little to no symptoms until your vision is affected. These cloudy spots can make it difficult to enjoy the activities you love as well as interfere with daily tasks like driving and reading.
A healthy lens lets light pass through the eye and focuses it on the retina, similar to a camera. Over time the lens becomes thick, less flexible, and clouded, causing your vision to become blurry and muddled. This is a natural part of growing older, but diabetes can accelerate their growth and cause them to develop much sooner than they normally would.
There are a few important factors that can cause you to develop diabetes-related cataracts. These include:
- How long you’ve had diabetes
- How often your glucose levels have been above target range
- The presence of diabetic macular edema
It’s important to keep in mind that cataracts are a natural part of aging and most people will develop them at some point. However, diabetics should be extra cautious to control their blood sugar to prevent them from developing sooner than normal.
Cataract Symptoms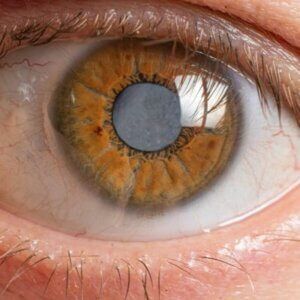
Cataracts have common symptoms whether they’re caused by diabetes or not. Common cataract symptoms include:
- Blurry or clouded vision
- Double-vision in one eye
- Seeing halos around lights
- Sensitivity to light and glare
- Poor vision at night
- Colors appear washed out
Cataract Treatment
There are multiple treatments for cataracts depending on their severity. Surgery is usually reserved as a last-case scenario with less invasive treatments being preferred. This can include:
- A stronger eyewear prescription
- Wearing anti-glare glasses and sunglasses
- Brighter lighting in your home and office
- Magnifying glasses
Cataracts usually develop slowly so the above treatments can work for a long period of time. However, cataract surgery may eventually be necessary. In this procedure, the old lens is surgically removed and replaced with a new intraocular lens . This new lens is crystal clear, allowing you to see like you once did without any effects of cataracts.
Intraocular lenses can vary from standard lenses, which help with up-close or distance vision, to toric lenses and multifocal lenses. Toric lenses can help with astigmatism as well as either up-close or distance vision. Multifocal lenses are the most advanced and can address all of your refractive issues post-surgery.
Are you suffering from a form of diabetic eye disease? Contact us today to schedule an appointment and get the treatment that you need!
Diabetic eye disease is an umbrella term for a variety of eye diseases related to diabetes. The best way for your ophthalmologist to spot these diseases and provide treatment is through comprehensive eye exams. Common diabetic eye diseases include early and advanced diabetic retinopathy, diabetic macular edema, glaucoma, and cataracts.
Baptist Eye Surgeons is an ophthalmological practice in Knoxville, TN, and Morristown, TN. Give us a call at 865-579-3920 for more information or to schedule an appointment .