5 Types of Eye Infections That You Should Be Aware Of
Eye infections affect millions of Americans per year and can often require a visit to the doctor. Although they may have similar symptoms, infections vary in their causes. This can include bacterial or fungal infection, a virus, or even caring for your contacts improperly.
Common types of eye infections include:
- Conjunctivitis (pink eye)
- Keratitis
- Cellulitis
- Shingles
- Endophthalmitis
It’s important to know the signs of an eye infection so you can contact our office immediately. Our ophthalmologists will be able to diagnose what kind of infection it is and develop a treatment plan to make you feel comfortable as well as protect your vision.
1. Conjunctivitis (Pink Eye)

Conjunctivitis occurs when the clear layer that covers your eye and lines your eyelid (the conjunctiva ) becomes infected or inflamed. This causes the small blood vessels in the membrane to become more visible, resulting in the whites of your eyes taking on a pink or reddish color.
The infected eye or eyes may also feel itchy or gritty. You may experience more tearing as well as discharge. This discharge turns into a crust overnight and can make it difficult to open the affected eye or eyes in the morning.
Also known as pink eye , conjunctivitis has two main causes — a viral infection or bacteria. Most cases are the result of viral infection , specifically of the adenovirus which causes many cold-like symptoms.
However, viral cases can also be caused by the:
- Varicella-zoster virus
- Herpes simplex virus
- Coronavirus
Bacterial conjunctivitis is rarer, but more likely if you wear contacts. For instance, wearing contacts overnight or using someone else’s contacts can result in a bacterial case of pink eye.
How to Prevent Pink Eye
Both bacterial and viral conjunctivitis are contagious so it’s important to know how to protect yourself and your family members. Symptoms often coincide with a cold or respiratory infection, so you need to be on high alert during the winter months.
To prevent getting pink eye, make sure that you and your family are:
- Not touching your eyes with your hands
- Washing your hands regularly
- Using clean washcloths and towels
- Not sharing washcloths and towels
- Changing your pillowcases
- Not sharing eye makeup or other personal care products
Good hygiene is key for preventing pink eye, so make sure that you and your loved ones are taking every precaution to avoid it. While it’s no more contagious than the common cold, following these steps will drastically reduce your risk of catching it.
Click here to learn more about why pink is more common during cold and flu season.
2. Keratitis
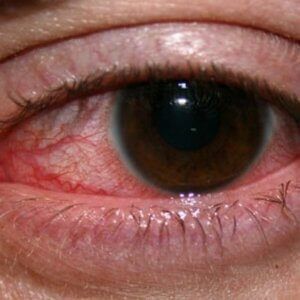
Inflammation of the cornea , the dome-shaped layer covering the iris and pupil, is known as keratitis . This can cause your cornea to become red and irritated, much like conjunctivitis.
Other symptoms include:
- Eye pain
- Increased tear production
- Discharge from the eye
- Difficulty opening your eye due to irritation or pain
- Blurry or decreased vision
- Sensitivity to light
- Feeling like something is stuck in your eye
It’s important to schedule an appointment with us immediately if you suspect you have keratitis. Failure to seek treatment can result in corneal scars, sores, and recurring infections. Temporary blindness and vision loss can also occur without treatment.
Keratitis can occur for a number of reasons. Viral keratitis is usually caused by the herpes simplex or herpes zoster viruses. Bacterial keratitis can be the result of contaminated contact lenses. These cases of infection can be caused by bacteria, fungi, and parasites that grow on the surface of your contact lenses or their carrying case. Make sure that you’re wearing your contact lenses as prescribed and not wearing them longer than directed.
You can also develop bacterial keratitis from contaminated water in oceans, rivers, lakes, and hot tubs. This type of infection is rarer since the cornea needs to have broken down in some way beforehand, such as wearing contact lenses for longer than directed. If this is the case, bacteria can enter your eye while swimming in contaminated water.
Who’s at Risk for Keratitis?
Some people have a higher risk of keratitis than others. This includes those who:
- Wear contact lenses
- Have a weakened immune system
- Use corticosteroid eye drops
- Have experienced an eye injury
People who wear contact lenses should be extra careful to take care of them. Contact lenses can be a breeding ground for bacteria, so make sure that you’re cleaning them correctly and not wearing them while swimming. You should also never sleep in your contacts since this can weaken your cornea. Consider daily contacts to avoid this problem.
Those with a weakened immune system are also at a higher risk for keratitis. You can have a weak immune system for different reasons, including disease and even taking certain medications. Talk to one of our surgeons about your risk and what you can do to protect yourself from an eye infection.
Talk to your eye doctor if you use corticosteroid eye drops since they can increase your risk of keratitis or even make your symptoms worse if you have an infection. Those who have experienced an eye injury involving the cornea may be at a higher risk for keratitis in the future.
Preventing Keratitis
Proper cleaning and wear are of the utmost importance if you wear contact lenses . To help keep your contacts in perfect condition, make sure to:
- Wash and dry your hands thoroughly before handling them
- Only use sterile products made specifically for your contact lenses
- Rub your contacts gently when cleaning to get rid of as much bacteria as possible
- Replace your contacts every three to six months or when instructed
- Never reuse contact solution
- Take your contacts out when you go swimming
- Follow any instructions your eye doctor gives you for cleaning and wearing them
For the best protection, consider switching to daily contact lenses. They’re designed to only be worn once, which drastically reduces your risk of eye infection due to contact lenses.
Viral keratitis can’t always be prevented. However, there are a few steps you can take to help keep their occurrences low.
- Wash your hands regularly throughout the day to avoid viral outbreaks
- Avoid touching your eyes, eyelids, or the skin around your eyes if you have a cold sore or blister. Make sure to thoroughly wash your hands first if you must.
- Only use eye drops that have been prescribed by your eye doctor
By following these tips, you’ll help protect yourself and those around you from keratitis outbreaks.
Click here to learn more about the dangers of swimming while wearing contacts!
3. Cellulitis

Cellulitis is an infection within the tissue of your skin. It’s most common in the legs and arms but can also occur around the eyes. While it’s possible for this infection to develop in healthy skin, it usually occurs following a break in the skin, such as a cut or following surgery. Bacteria uses the break in the skin to enter the body and cause an infection.
There are different types of bacteria that can cause cellulitis , with the most common being:
- Hemolytic streptococcus
- Streptococcus pneumoniae
- Staphylococcus aureus
Hemolytic streptococcus and streptococcus pneumoniae are forms of strep while staphylococcus aureus is a form of staph infection. Both are common culprits for infections around the nose and mouth. However, it’s also possible to get an infection from animal bites and injuries that happen while in water.
Symptoms for cellulitis can vary, but cellulitis around the eye has a few tell-tale signs . This usually includes redness around the eye or in the white of the eye. It’s also common for the eyelid, whites of the eye, and the surrounding area to become swollen. The affected area will also feel tender.
Other symptoms include:
- Fever
- Chills
- Headache
- Weakness
- Blisters
Seek medical treatment immediately if you experience numbness, tingling, or if the affected skin turns black. Those with diabetes or who have weakened immunity should also see their doctor as soon as possible.
Diagnosing Cellulitis
Cellulitis can be mistaken for other skin conditions so it’s important to get a diagnosis from your eye doctor. We usually base our diagnosis on your medical history and physical exam. Blood and skin samples may be taken to confirm your diagnosis. This also helps to identify the type of bacteria involved and come up with the best treatment for your case.
Treating Cellulitis
Treatment for cellulitis is based on your age, overall health, and the severity of your case. Seeking treatment early helps ensure that the infection doesn’t spread to your eye socket.
These treatments may include:
- Antibiotics (oral, topical, injection, IV)
- Cold compresses on the affected area
- Cleaning the area and keeping it dry
You’ll also need plenty of rest and time to heal. In some cases, surgery may become necessary.
Preventing Cellulitis
Caring for your skin is the best way to prevent cellulitis. This includes:
- Bathing regularly
- Washing your hands
- Wearing gloves and footwear to prevent cuts and scrapes
- Keeping dry skin moisturized with lotion
Make sure to clean the wound if you have a break in your skin. Apply some antibiotic ointment and keep it covered with a bandage. Keep an eye on it for signs of infection.
Those with diabetes should pay special attention to breaks in skin or infection. You should also refrain from cutting calluses and warts, as well as cutting your nails too short.
Click here to learn more about the connection between swollen eyelids and cellulitis!
4. Shingles

Shingles are caused by a viral infection resulting in a painful rash. They’re most prevalent around your torso, but they can also occur around the eye. You should contact your doctor if you think you have shingles, but shingles around the eye can be especially dangerous since it can lead to serious vision problems.
Shingles is a result of having had chickenpox at some point in your life. The varicella-zoster virus , which causes chickenpox, remains in the body once chickenpox has gone away. The virus lays dormant in some people but can become active again in others, resulting in shingles. This can happen multiple times over a person’s lifetime.
The first symptom of shingles, also known as herpes zoster , is usually pain. This can manifest as a dull throbbing for some, but others may experience a burning or stabbing sensation. The pain from shingles can come and go. A rash in the form of tiny blisters is another common symptom of the infection.
Other symptoms of shingles in or around the eye include:
- A burning sensation
- Sensitive skin
- A red rash
- Blisters forming on the upper eyelid
- Swelling and redness around the eyelid
- Blurred vision
- Sensitivity to light
- The eye feeling irritated and itchy
These symptoms are also common in other types of eye infections so consult your eye doctor for a correct diagnosis. An eye infection requires immediate medical attention, but complications from shingles can be even more severe since they can cause inflammation, corneal ulcers, and glaucoma.
The shingles virus exists in sensory nerves which is why the pain can be so severe. Sometimes it can affect your facial nerves specifically, resulting in eye-related symptoms.
Treating Shingles of the Eye
Shingles of the eye can result in vision loss so it’s extremely important to seek immediate medical attention. It can be diagnosed with a physical exam, but fluid samples from the blister may be taken for testing. This helps determine if it’s the shingles virus and what kind of treatment you need.
Antiviral medications will be prescribed upon diagnosis. These are available in tablet and liquid form and should be taken immediately to help combat the infection. Those with a weakened immune system may have to be admitted to the hospital for IV treatment. We may also recommend anti-inflammatory eye drops to dilate the pupil and fight inflammation.
Who’s at Risk for Shingles?
The Center for Disease Control (CDC) estimates that 1 in 3 Americans have shingles. Anyone who has had chickenpox can develop the infection, but it’s much more common in people over the age of 50.
Experts aren’t certain what actually reactivates the virus, but risk factors include:
- Being under a lot of stress
- Having another form of illness
- Having a weakened immune system
- Being older
Talk to your doctor about your risk factors for shingles and what can be done to prevent them from developing.
Complications
It is possible for shingles to go away on their own. However, the possible complications mean you should seek medical treatment immediately.
The most common complication is pain that lasts for three months after the rash appears ( postherpetic neuralgia ). Other possible complications include:
- Glaucoma
- Retinal necrosis (which can cause blindness)
- Corneal ulcers
- Scarring
Shingles can be especially dangerous during pregnancy since a fetus can contract the virus through the blood. This can be especially dangerous for infants that are born prematurely since they face an increased risk of complications.
Prevention
The best way to prevent shingles is through vaccination. It’s recommended that people over the age of 50 be vaccinated due to it being more common in older adults and the severity of possible complications.
You can minimize the risk of spreading shingles by:
- Keeping rashes covered
- Not scratching it
- Practicing good personal hygiene
- Washing your hands after touching the rash
Shingles is contagious so it’s important to quarantine yourself if you have it. This is especially important for protecting people who have never had chickenpox. You’ll know you’re no longer contagious when the blisters have healed, which can take anywhere from two to four weeks. People who catch the virus will develop chickenpox instead of shingles.
5. Endophthalmitis
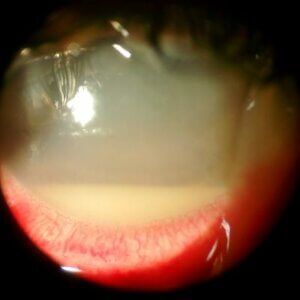
An infection of the fluids or tissue inside the eye is known as endophthalmitis. These infections can result in blindness, so it’s important to seek medical treatment immediately in order to preserve your vision.
Endophthalmitis comes in two main forms :
- Exogenous endophthalmitis
- Endogenous endophthalmitis
Exogenous endophthalmitis is the more common of the two. In this case, the infection comes from outside the body, usually from a puncture wound. This could be due to fungi or bacteria that get in the eye after surgery, an injection to the eye, or an eye injury. Symptoms usually begin a few days after a surgical procedure or injury.
Quickly developing cases are known as acute endophthalmitis . Symptoms that take longer to develop are known as chronic endophthalmitis . These cases are often caused by specific forms of bacteria and fungi.
Endogenous endophthalmitis is caused by an infection that spreads to the eye from another part of the body. This could be due to a blood or urinary tract infection.
Both types of endophthalmitis have similar symptoms, including:
- Eye pain that gets worse after surgery, injection, or injury
- Redness in the eye
- Discharge from the eye
- Eyelids that are puffy or swollen
- Blurred, decreased, or lost vision
Diagnosis & Treatment
Your eye doctor will perform a series of tests to determine if you have endophthalmitis, including an eye exam and testing your vision. They will also want to know about any recent eye procedures or injuries to determine if they might be the cause. They may recommend ultrasound in the case of injury to check for any foreign objects in your eye.
An aqueous/vitreous tap test may be used if your eye doctor suspects an infection. It involves taking a fluid sample from your eye with a tiny needle, which is sent to a lab for testing.
Treatment for endophthalmitis involves injecting antifungal or antibiotic medicine into the eye. Steroids may also be used to reduce inflammation and swelling from injections. Vitrectomy surgery may be necessary for severe infections. In this procedure, the gel is removed from your eye followed by an injection of medicine.
Preventing Endophthalmitis
You can help prevent endophthalmitis by:
- Wearing protective eyewear during housework and other activities that threaten your eyes
- Wearing protective eyewear during contact sports
- Making sure to follow your doctor’s instructions following an eye injection or eye surgery
Following these tips can help to greatly reduce the risk of bacteria and fungi entering your eye and causing an infection.
Do you need treatment for an eye infection? Contact us today to schedule your appointment!
Eye infections are a common occurrence that are easily treated, especially in their early stages. They can happen for a variety of reasons, whether it’s from an injury, virus, or wearing your contacts for too long. Contacting your eye doctor immediately can help get rid of uncomfortable or even painful symptoms, as well as protect your eyes from vision loss and other complications.
Baptist Eye Surgeons is an ophthalmological practice in Knoxville, TN, and Morristown, TN. Give us a call at 865-579-3920 for more information or to schedule an appointment .